Ear Infections: Symptoms, Treatment, and When to Visit
March 16, 2026
Ear infections are one of the most common reasons people walk into our clinic — especially parents with young children. That nagging ear pain, the muffled hearing, the child who will not stop tugging at their ear at two in the morning. If any of that sounds familiar, you are not alone. According to the National Institute on Deafness and Other Communication Disorders (NIDCD), ear infections are among the most frequent reasons for pediatric doctor visits in the United States.
Here is what you should know about ear infections — what causes them, how to recognize the symptoms, and when it is time to come in rather than wait it out.
What Causes Ear Infections?
An ear infection happens when bacteria or viruses cause inflammation and fluid buildup in the ear. There are two main types, and they are quite different:
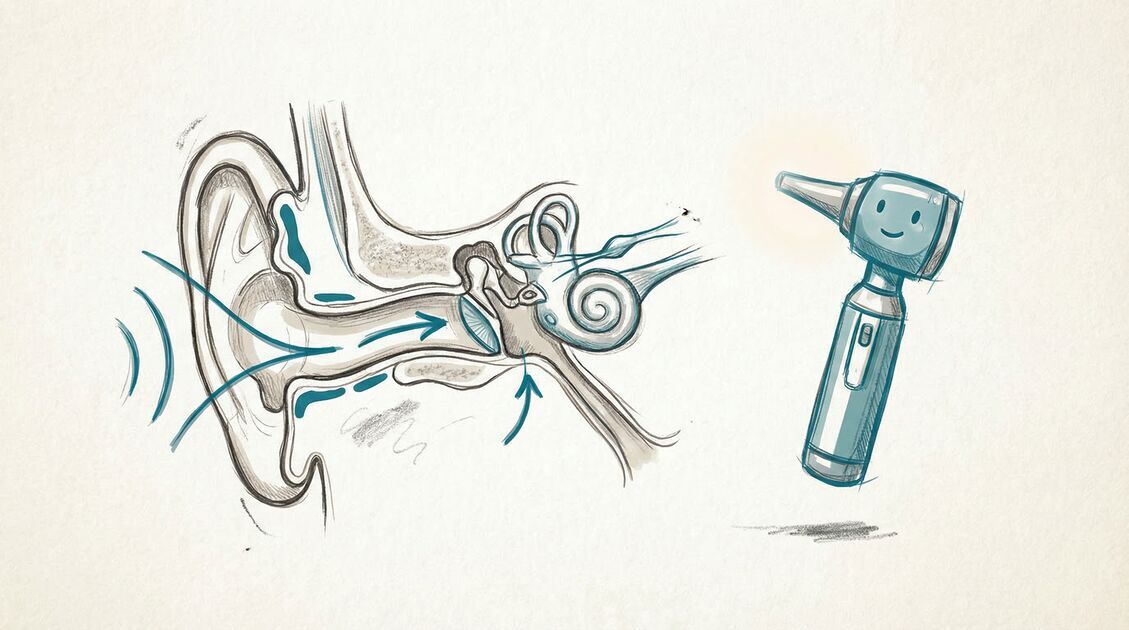
- Middle ear infections (otitis media). This is the type most people think of, especially with children. It occurs behind the eardrum, usually following a cold or upper respiratory infection. Swelling and congestion block the eustachian tube — the narrow channel connecting the middle ear to the back of the throat — and fluid gets trapped. That warm, stagnant fluid becomes a breeding ground for bacteria. According to the CDC, middle ear infections can be caused by both bacteria and viruses, which matters when it comes to treatment decisions.
- Outer ear infections (otitis externa or swimmer’s ear). This type affects the ear canal — the passage from the outer ear to the eardrum. It is commonly triggered by water that remains in the ear after swimming or bathing, creating a moist environment where bacteria thrive. Scratching or inserting objects into the ear canal can also cause it.
Symptoms in Adults
Adults with a middle ear infection typically experience:
- Ear pain — a dull ache or sharp, stabbing sensation
- Muffled hearing or a feeling of fullness in the ear
- Fluid drainage from the ear
- Mild fever
With swimmer’s ear, the symptoms are a bit different: itching inside the ear canal, redness, discomfort that worsens when you tug on the outer ear, and sometimes swelling or drainage. The pain with outer ear infections often gets worse over a few days if untreated.
Symptoms in Children
Young children cannot always tell you what hurts, so you have to watch for behavioral cues:
- Pulling or tugging at the ear
- Increased fussiness or crying, especially when lying down
- Difficulty sleeping
- Trouble hearing or not responding to quiet sounds
- Fever (100.4°F or higher)
- Loss of appetite — swallowing can be painful with a middle ear infection
- Fluid draining from the ear
Why Do Kids Get Ear Infections So Often?
If it feels like your child gets ear infections constantly, there is a good anatomical reason. Children’s eustachian tubes are shorter, more horizontal, and narrower than those of adults. That means fluid does not drain as easily from the middle ear, and blockages happen more readily during colds and allergies. The NIDCD notes that most children will have at least one ear infection by their third birthday. As children grow, their eustachian tubes lengthen and angle more steeply, which is why ear infections become less common with age.
Children in group daycare settings are also at higher risk because they are exposed to more colds and respiratory viruses, which often trigger middle ear infections.
Watchful Waiting vs. Antibiotics
Not every ear infection needs antibiotics — and this is an area where the guidelines have evolved over time. The American Academy of Pediatrics (AAP) otitis media guidelines recommend a “watchful waiting” approach in certain situations:
- Children 6 months to 2 years with mild symptoms and a single affected ear
- Children 2 years and older with mild symptoms in one or both ears
- Adults with mild, uncomplicated infections
Watchful waiting means monitoring symptoms for 48 to 72 hours while managing pain at home. Many ear infections — particularly those caused by viruses — will resolve on their own during this window. The CDC emphasizes that prescribing antibiotics when they are not needed contributes to antibiotic resistance, which is a growing public health concern.
However, antibiotics are typically recommended right away when:
- The child is younger than 6 months
- Symptoms are severe (high fever of 102.2°F or above, significant pain)
- Both ears are infected in a child under 2 years
- There is ear drainage (which can indicate a ruptured eardrum)
- Symptoms do not improve or get worse after 48 to 72 hours of observation
Your provider will evaluate the specific situation and recommend the best course of action. When antibiotics are prescribed, it is important to finish the full course even if symptoms improve before the medication is gone.
Managing Pain at Home
Whether you are in a watchful waiting period or waiting for antibiotics to take effect, there are several ways to keep pain under control:
- Over-the-counter pain relievers. Acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) can reduce pain and fever. Follow dosing guidelines for age and weight, especially for children. Do not give aspirin to children.
- Warm compress. A warm, damp washcloth held against the ear can ease discomfort.
- Elevate the head. For children old enough to sleep with a pillow, keeping the head slightly elevated can help fluid drain and reduce pressure.
- Stay hydrated. Swallowing helps open the eustachian tube, so encourage plenty of fluids.
Avoid putting anything inside the ear — no cotton swabs, no drops unless specifically prescribed by a provider.
When to See a Doctor
Some ear infections resolve on their own, but certain signs mean you should come in promptly:
- Pain that persists beyond 2 to 3 days or is severe from the start
- Fever above 102.2°F in a child, or any fever in an infant under 3 months
- Fluid or pus draining from the ear
- Hearing loss that does not improve as other symptoms clear up
- Symptoms that return shortly after finishing antibiotics
- Recurrent infections — three or more episodes in six months, or four or more in a year
For swimmer’s ear, see a provider if pain or swelling is worsening, if you have diabetes or a weakened immune system, or if home treatment has not helped after a day or two. Outer ear infections typically require prescription ear drops to clear up properly.
Quick, Thorough Care for Your Family
Ear infections are uncomfortable, and when they happen to your child, the worry makes it worse. The good news is that most ear infections are straightforward to diagnose and treat. A provider will look inside the ear with an otoscope, assess the eardrum and any fluid, and determine whether antibiotics, prescription ear drops, or continued observation is the right call.
At Covenant Clinic, we see patients of all ages for ear infections — from toddlers to adults. We are open 7 days a week, 7:30 AM to 7:30 PM, and you do not need an appointment. Walk in, and we will take care of it.
Dealing with ear pain right now? Save your spot online or walk in to Covenant Clinic at 3961 E Lohman Ave, Suite 34, Las Cruces. You can also call us at 575-556-0200 with any questions.